Like a ship that runs aground because of low tide or unseen rocks or fog or navigational errors, our beautiful heart can be damaged when blood flow is restricted or when it flows unregulated.
Heart/wrecked.
I grew up hearing the term, “Stress kills.”
I was never quite sure what that meant, but then I did when it happened to me.
After a seemingly nonstop barrage of a personal stressful situation–like a ship hitting the rocks over and over again–it all finally took an undeniable toll on my physical health.
One of my favorite places to live is in the state of Denial, but I’ve been forced to temporarily move to a new town called Reality. Hopefully, I’ll just visit there for a bit until I can come home again.
After experiencing some intermittent and strangely terrifying heart pains, I went to the doc who took my blood pressure and was concerned about the results. It was super high. I had always had enviably LOW blood pressure since I exercise regularly, am vegan and never smoked, so this raised concerns.
Over the course of a couple weeks, my BP was checked daily and it stayed consistently high; dangerously high, which only made me more anxious and more stressed, and at one of the office visits, I started hyperventilating and had a panic attack. (Super embarrassing for the doc and absolutely mortifying for me.)
This led to an order for an Echocardiogram along with all the other heart-focused tests. The echo was done at a local hospital–a definite trigger. No one wants to go to a hospital at any time, but especially during Covid. It seemed like I was being admitted, with a wrist band and lots of little stickers, and I was devastated.
I almost bolted out of the front door at that point, but I persevered. I can share with you that it’s a scary time when you have to figure out why you don’t feel great. I’ve been a medical advocate for several loved ones, but it’s radically more difficult when you have to care for yourself. Poor me.
The technician was amazing, especially considering I tormented her with a million questions. I know enough about medical stuff to see that she was concentrating on a certain area of my heart. I really appreciated her patience with me and her detailed explanations during the hour-long ordeal.
The results showed a dilated aortic root valve and regurgitation of the mitral valve.
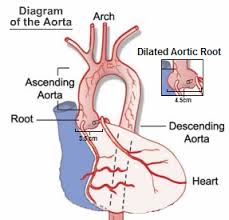
What this means is that the accumulation of stress and panic attacks and PTSD that I’ve endured during the last four years manifested medically and physically and caused structural damage to my heart.
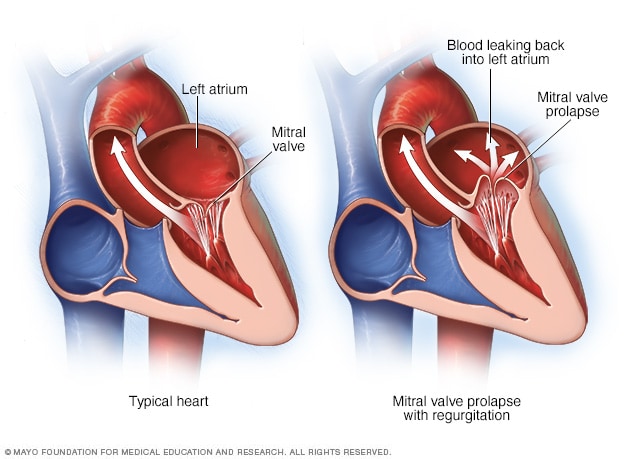
“Severe physical or emotional stress increases blood pressure to the point where the tensile limit of the aortic tissue is overwhelmed, causing the rupture.”
“Over time, certain conditions, such as high blood pressure, can cause your heart to work harder, gradually enlarging your heart’s left ventricle.”
“Mitral valve regurgitation can cause complications such as atrial fibrillation, in which the atria of the heart don’t contract well. This leads to increased risk of stroke. Also, elevated blood pressure in the lungs (pulmonary artery hypertension).”
Hypertension makes the blood push harder against the valve and causes it to dilate, enlarge, and that’s pretty much the same scenario for the mitral valve, which seems to be the cause of the intermittent chest pain.
I’ll need to be monitored regularly because if I can’t control the stress/blood pressure and the valves stretch to a dangerous size, the only solution is surgical intervention–or death.
Reducing stress and hypertension can possibly keep the valves from enlarging any further, but the damage is done–nothing will make them reduce in size back to normal, except surgery.
Let me tell you that it’s true. Stress kills.
Now I’m off to change course, take some magnesium, eat more beets, meditate, calm down and regulate my breathing so that I don’t have a stroke or an aneurysm.

Heart/wrecked.
Shipwrecked.